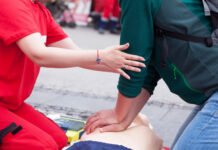
The pulse oximeter, which can be used for assessing the oxygen position of patients in many different clinical settings, is now an increasingly common article of monitoring equipment. It gives constant, nonstop observation of oxygen saturation of haemoglobin in blood glucose. Its effects are updated with every pulse wave. They do, however, provide a chance for deviations from an individual’s oxygen evaluation to be detected quickly, as an early warning sign to clinicians to help stop the outcome of desaturation and discover hypoxaemia until it generates cyanosis. It’s been indicated that the gain in the use of pulse oximeters generally wards could see it becoming as commonplace as the thermometer. However, employees are reported to have limited instruction in the functioning of the apparatus and limited understanding of how it functions and what factors can influence the readings. This paper intends to promote a better awareness of the value of getting the suitable knowledge base prior to using pulse oximetry and also to supply a supply of reference and education to teaching purposes.
How does the pulse oximeter work?
Of light from oxygenated haemoglobin when compared with that of decreased haemoglobin. Arterial oxygenated blood is red because of the caliber of oxyhaemoglobin it comprises, causing it to absorb light of particular wavelengths. The oximeter probe includes two light-emitting diodes (LEDs), one red and one infrared, situated on either side of this probe. The research is set on a suitable region of the human body, normally a fingertip or ear lobe, and the LEDs transmit light wavelengths through pulsating blood flow into a photodetector on the opposite side of this probe. Infrared light is consumed by the oxyhaemoglobin; reddish light from the decreased haemoglobin. Pulsatile arterial blood during systole induces an influx of oxyhaemoglobin into the tissue, consuming more infrared light, and letting less light to reach the photodetector. The outcome is processed into an electronic screen of oxygen saturation to the oximeter display, which can be symbolised as SpO2. There are various models and makes of pulse oximeters accessible most supply a visual electronic waveform screen, an audible screen of arterial pulsations and heart rate, and a number of detectors to accommodate people irrespective of age, weight or size. Choice is dependent upon the surroundings where it’s used. All employees working with the pulse oximeter has to know about its functions and proper usage. Arterial blood gas analysis is much more precise; nonetheless, pulse oximetry is considered sufficiently accurate for many clinical purposes. For taking best readings you should have best pulse oximeters.
Factors which affect accuracy of readings
Patient Illness – To figure out the difference between empty and full capillaries, oximetry measures light absorption over a variety of pulses, normally five. For a pulsatile leak to be discovered, there has to be adequate perfusion from the monitored location. If the individual has a weak or absent peripheral heartbeat, pulse oximeter readings won’t be precise. Patients at risk of non perfusional conditions are individuals with hypotension, hypovolaemia and hypothermia and people in cardiac arrest. Patients that are chilly but not hypothermic might have vasoconstriction within their hands and feet that can also undermine blood circulation. Non-arterial stimulation may be discovered if the research is procured too. Gradually, producing venous pulsations from the finger. Cardiac arrhythmias can cause quite inaccurate measurements, intravenous dyes utilized in diagnostic and haemodynamic testing might using pulse oximetry properly involves more than simply studying the amount screen, because not all patients with the exact same SpO2 possess the exact same amount of oxygen into blood. A saturation of 97% means 97% of those total quantity of haemoglobin in the entire body is full of oxygen molecules. Thus the interpretation of oxygen saturations has to maintain the context of the patient’s complete haemoglobin level. Another element that affects the oximeter may change with different physiological problems.